Cataract Story
Anna-bo
The Cosmic Raccoon

7 Year Old Chocolate Lab
Thump! Thump! Thump! Thump! Thump! Thump! Thump! Thump! Thump!
Scraaaaaaaaape!
Crash! Bang! Clomp!
These are the sounds of the Cosmic Raccoon out for a walk. Lots of picket
fences to thump her E-Collar on. Nose to the sidewalk, scraping the
collar
as she goes. Cat smell . . . Bang! Where did that tree come from?

The second I saw her shaved eye mask and E-Collar,
Anna became the Cosmic Raccoon.
Poor thing. She had a false start on surgery a couple of months ago.
Got
sedated and then Dr. Gratzek decided after looking at her eyes one
more time
that she wasn't yet ready. We have heard the horror stories of
rapidly-progressing cataracts, but Anna's, which I noticed more than
eight
months ago, just weren't getting worst. After the false start, we came
by
for weekly check-ups and Dr. G. gave me her pager number so I could
contact
her if I noticed any change in Anna's eyes.
If anything, she seemed much better this year
at catching flies, but having had a blind dog,
I know that they can do some pretty amazing things even if they can't
see.
Anna was on topical prednisolone the week before both her scheduled
surgeries.
This drove her BG's up to a point where we had to increase her insulin
from 11 units to 15.
As usual, she was a golden angel when it came to letting me put the
Voltaren
and pred in her eyes. That's not to say that she wouldn't have a sudden
urge
to shake her head, scratch her ear or do something else that sent the
drop
of medicine intended for her eyes somewhere else. She does the same
with her
insulin shot. She always comes to me, sits and is great about the shot,
but
is very easily distracted. When I bend over, she assumes I must be
inviting
her to give me a big, slobbery kiss. When I grab her head for the eye
drops,
she just knows deep down that I really want to give her a big tummy
rub.
She's a Bo-bo Girl after all.
The day of surgery, Dr. G. reiterated that if Anna was in any way stressed
after the surgery, I would have to take her home. She went over what
that
meant in terms of eye drops every two hours and a whole pharmacy worth
of
medicines. As much as I love Anna, I hoped that the sedation would
keep her
calm and she could stay at the hospital for that critical first 24
hours following surgery.
We arrived at the veterinary hospital early, well not really. Guess
I should
explain. We arrived promptly at 8:25am so as not to be late for our
8:30am
scheduled arrival. Old East Coast habits die hard. I know this is Santa
Cruz
where time is about half way between Pacific Standard Time and manñana.
The
receptionist arrived around 9am, the nurses and Dr. G. sometime after.
This
is an important part of the story because Anna is a bit too enthusiastic
to
sit around quietly in a veterinary waiting room. She greets each new
patient
with loud barks and strains at her leash to go see them.
This meant we had to walk round and round the hospital parking lot for
almost an hour, something with later consequences for her recovery.
Once Dr. G. arrived, she re-checked Anna's eyes and said she felt very
good
about surgery. The nurse wanted to take the Bo-bo Girl back to a kennel
where they could begin the pre-op regime of eye drops and sedation,
but
knowing Daddy's little girl, I suggested heavy sedation if she didn't
want
Anna barking loudly and disturbing everyone.
And knowing Anna, Dr. G. instructed the nurse to up the dose a bit.
About 15 minutes later, Anna was staggering around like a sailor on
shore
leave after 6 months at sea, but when the nurse tried to escort back
to the
kennel, my little girl weighed several tons and wasn't about to leave
me.
The nurse handed me the leash and I followed back to a nice big kennel.
Anna was so out of it that she fell asleep in a few seconds.
I went home to rest up for what I knew was going to be a 24-hour ordeal.
As much as I hoped Anna could stay, I knew it wasn't going in the cards.
Surgery got postponed because of an emergency so it wasn't until 4pm
that
Dr. G. called. She sounded panicked. "Get right down here. You are
going to
have to take Anna home. She is loaded with anesthesia and gallons of
sedative, but she's barking, whimpering and struggling to get out of
the
kennel. I've got two nurses with her, but hurry."
That's my girl.
I was greeted by Dr. G. and one of her nurses who were rapid fire giving
me
instructions for all Anna's meds. Since they were writing them down,
I
didn't listen. Meanwhile, I could hear the Bo-bo Girl barking in the
back.
And then there she was, staggering down the hall at the limits of her
leash
and with a steady stream of PEOPLE TALK, a valiant attempt to speak
my
language that is somewhere between the sound of a gaggle of geese and
a
grunting sound.
She looked so sad with her shaved eye mask and E-Collar. Once she reached
me, she collapsed in a classic Chocolate Melt, E-collar resting on
my foot
and leg. She was out of it.
It took some help to get her in the car where instead of sleeping, she
insisted on trying to stick her head out the window, all the while
squinting
narrowly in the bright afternoon California sun.
At home, she again lost all her energy. I managed to get her out of
the car
and in the back gate, but then she came to and her big brother Murphy
had to
investigate what had happened to Anna with his nose.
I tried getting her up and into the house, but she was out of it so
rather
than fight it, I let her stay where she was in front of the door.
When it was time for her first set of drops, I had to do one side, roll
her
over and do the other. She wouldn't sit up. But she did spit up.
About that time, Dr. G. called to say that Anna had vomited when the
induced
her. That surprised me because it had been close to 15 hours since
she ate.
I later found out that some of the students I share my house with had
dumped
a big Greek salad in my compost heap rather than the compost bin and
Anna
must have eaten the whole thing.
She remained out of it for close to 36 hours. She didn't drink and wasn't
interested in eating--an all time first for the Bo-bo Girl.
For the most part, she seemed comfortable, but she fought the E-Collar
horribly and managed to get it off three times. I tightened her collar
one
more notch each time and was worried that she wasn't going to be able
to
breath if I tightened any more.
The next morning, we went off to see Dr. G. The newly dubbed Cosmic
Raccoon
was still pretty groggy, even walked all the way through the waiting
room
without barking at the other dogs and cats.
Dr. G. checked her pressures. They were perfect at 11.
The sutures were still in place and all was well.
I told her that Anna was going nuts fighting the E-Collar and Dr. G.
got to
see it herself. She was scratching at her ear and trying to bite at
her back
leg through it.

It hadn't occurred to me that it could be fleas. It was Dr. G's first
thought.
She rolled Anna on her back and there on her little tummy was a shimmering
mass
of fleas which I have to assume she picked up while we walked around
the hospital
parking lot before surgery. I had just bathed her the day before and
because
Murph was having an allergic dermatitis attack had checked both
very carefully for fleas. Murph had even been inspected by our regular
vet.
After checking with Dr. G and Dr. B, Anna's internist, I gave her some
Front-line for the fleas and then applied my magic flea medicine to
her
stomach until I couldn't see any more fleas. I have no idea what led
me to
think it would work, but many years ago after a weekend hike when both
dogs
were covered in fleas, I mixed up a concoction which was about half
alcohol
and half an Aloe hand cream.
I have no idea why it works, but if I soak a face cloth in this mixture,
I
can literally wipe the fleas off the dogs. It doesn't get every one
so after
wiping her tummy, legs and elsewhere, I then just sat down and started
pulling them off one by one, sitting on the bathroom floor with Anna
and
dumping them into the toilet.
By the next day, Anna was Anna. She has completely forgotten about her
E-Collar and is resigned to sitting quietly for her eye drops and ointment.
We have an agreement that if the drop hits her face, we'll count it.
We are down to two drops and one ointment now every 6 hours. She was
supposed to have gone on Rimadyl and a variety of other oral medicines,
but
because her pressures were so good and her stomach a little upset,
we held
them. By the time of her second check-up, Dr. G. said to forget them.
At this point, she keeps showing off and reading the New York Times
at 20
feet and acting like a Bo-bo Girl. Dr. G. gave me a long list of Don'ts,
but
then just shook her head and said, "She's a Lab. I put in extra sutures."
Doing cataract surgery requires a major commitment of time at the beginning
and that needs to be taken into account in making a decision to go
forward
with it. The surgery itself is not without some risk of complications,
but
they seemed to me to be less than the potential problems that diabetic
cataracts could lead to untreated. I've had two blind dogs and know
that
blindness is not a problem for a dog if you just keep to a routine
and don't
let them become disoriented. But I worried about other problems from
diabetic cataracts and thought it best to do the surgery while she
was
healthy and there were no problems.
It is expensive, but if you are reading this, I know that you are part
of
the crowd who would mortgage your house to take care of your furbaby.
What can I say?
Edward Murray

Anna
Click here
to read Anna's Ninth Year Sugarversary Story!

Some cataract information from http://www.peteducation.com/
Cataracts
Joe Bodewes, DVM
Veterinary Services Department, Drs. Foster & Smith, Inc.
Cataracts are one of the most common problems affecting the eyes of
the dog. There are many different forms and causes of cataract formation.
They affect all breeds and ages of dogs but certain types show up more
commonly in certain breeds. Despite the fact that they are very common
there is still a lot that we don't know about canine cataracts. The only
current treatment option is surgery but with correct patient selection
the outcome is very good. This article will explain some of the different
forms of cataracts including their age of onset and their treatment
What are cataracts?
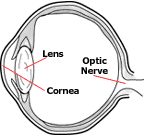
The word cataract literally means to break down. This breakdown refers
to the disruption of the normal arrangement of the lens fibers or its capsule.
This disruption results in the loss of transparency and the resultant reduction
in vision. Cataracts often appear to have a white or crushed ice appearance
and are found in the lens of the eye. |
 |
Nuclear sclerosis
I often get people that bring an older dog into the clinic complaining
of cataract formation in their dogs eyes. The vast majority of the time
the dog does not have cataracts but has the much more common condition
known as nuclear sclerosis. Nuclear sclerosis is a normal change that occurs
in the lens of older dogs. Nuclear sclerosis appears as a slight graying
of the lens. It usually occurs in both eyes at the same time and occurs
in most dogs over six years of age. The loss of transparency occurs because
of compression of the linear fibers in the lens. The condition does not
significantly affect the vision of the dog and treatment is not recommended.
How do cataracts form?
Despite the fact that there are several different forms and causes of
cataracts, they all develop in a similar fashion. The normal lens is maintained
in a dehydrated state. It consists of 66% water and 33% protein. There
is a complicated sodium water pump system in the lens that keeps this water/protein
balance in check. When the biomechanical system in the lens is damaged,
this pump system begins to fail and extra water moves into the lens. In
addition, the percentage of insoluble protein increases. These changes
result in the loss of transparency and cataract formation.
Age of onset
The age at which a dog develops cataracts is very important in classifying
the type of cataract. The age of onset is particularly important for determining
if the cataracts are the result of a hereditary trait in certain breeds
of dogs.
Congenital Cataracts: These are cataracts that are present at
birth. These cataracts usually occur in both eyes. Despite the fact that
the animal is born with them they are not necessarily inherited. Infections
or toxins may cause the formation of these cataracts while the puppies
are still in utero. Primary congenital cataracts such as those found in
miniature schnauzers are, however, inherited.
Developmental (Early Onset) Cataracts: Developmental cataracts
are those that develop early on in life. As with congenital cataracts they
may be inherited or caused by outside sources such as trauma, diabetes
mellitus, infection, or toxicity. Inherited cataracts at this age are
more common in several breeds including afghan hounds and standard poodles.
Senile (Late Onset) Cataracts: The cataracts that occur in dogs
over 6 years of age are called senile cataracts. They occur much less frequently
in dogs than in humans. Nuclear sclerosis, which is not considered to be
a medical problem, is often confused with cataracts at this age.
Inherited cataracts
Inherited cataracts in the dog may occur independently or in association
with other ocular disease. The breeds that appear to develop inherited
cataracts along with their age of onset are listed below. If a dog is diagnosed
with inherited cataracts, the dog should obviously not be used for breeding
because of the likelihood perpetuating the disease in the offspring.
| Breed |
Age of Onset |
| Afghan Hound |
6-12 months |
| American Cocker Spaniel |
6 + months |
| Boston Terrier |
Congenital |
| Chesapeake Bay retriever |
1 + years |
| German Shepherd |
8 + weeks |
| Golden Retriever |
6+ months |
| Labrador Retriever |
6+ months |
| Miniature Schnauzer |
Congenital or 6+ months |
| Old English Sheepdog |
Congenital |
| Siberian Husky |
6 + months |
| Staffordshire Bull Terrier |
6 + months |
| Standard Poodle |
1 + year |
| Welsh Springer Spaniel |
Congenital |
| West Highland White Terrier |
Congenital |
The most common metabolic disorder resulting in cataract formation in
the dog is diabetes mellitus. If diabetic dogs are followed for
a year or more, almost all of them would develop cataracts. In diabetic
dogs the glucose concentrations in the lens increases. The extra glucose
is converted into sorbitol, which causes an increase in the influx of water
to the lens. The increase in water causes a breakdown of the lens fibers
and a resulting cataract. Cataracts in diabetic dogs can develop extremely
rapidly if the dog is not regulated. They generally affect both eyes. Surgical
removal of the lens can be successfully performed in the diabetic dog if
the animal has been regulated successfully for at least three months.
Trauma
Trauma from an automobile accident, or penetration of a thorn, shotgun
pellet or other object may damage the lens and a cataract may develop.
These types of cataracts usually only occur in one eye and can be treated
successfully with surgical removal.
Treatment
Treatment for canine cataracts consists of surgical removal of the lens.
There is currently no good non-surgical treatment for this condition. With
the increase in veterinary surgical skill and equipment, the surgical procedure
to remove the problem lens is becoming increasingly more common. There
are several different techniques used to remove the affected lens including;
the removal of the entire lens and surrounding capsule, the removal of
the lens leaving the surrounding capsule, phacoemulsification of the lens,
and aspiration and dessication of the lens. All of these techniques can
offer excellent results. For a successful outcome the affected animal must
undergo a thorough examination to determine if it is a good surgical candidate.
Diabetic animals that are not regulated, aggressive animals that are difficult
to treat daily, or animals in poor or failing health, are not good surgical
candidates. If you suspect your dog is developing cataracts then you should
work closely with a veterinary ophthalmologist to take the best and most
effective course of treatment for the dog.
References
Gelatt. Veterinary Ophthalmology. Lea & Febiger. Malvern, PA; 1991.
Slatter, D. Fundamentals of Veterinary Ophthalmology. Saunders. Philadelphia,
PA; 1990.

These articles can be found at www.peteducation.com
This is one of the most up to date informative sites a pet owner can
bookmark
and research for information to help you in caring for your beloved
furchild!
© 2001 Drs. Foster & Smith, Inc.
Reprinted as a courtesy and with permission from PetEducation.com (http://www.PetEducation.com)
On-line store at http://www.DrsFosterSmith.com
Free pet supply catalog: 1-800-323-4208
|
More
Pet Diabetes Cataract Stories
Not all dogs will develop cataracts. Queenie is still cataract free
(touch wood)
and she has been a diabetic since April of 1995 which as of today's
date Sept. 5, 2001,
is six and a half years ago. Dr. Bob a month ago said he can still
see the back of her
retina perfect though she does have nuclear sclerosis. Nuclear sclerosis
can
be
mistaken by a vet for cataracts. My vet thought she had cataracts forming
originally and
she was immediately sent to an opthamologist. He diagnosed her with
nuclear sclerosis
which appears as a bluish gray haze on the lens of both eyes and is
common in older
dogs. Vision is not significantly affected by this so no treatment
is required.
|






